Substance use disorders in healthcare professionals are typically framed through behavioral, psychological, and social models.
These frameworks are essential—and have led to meaningful progress in awareness, treatment, and support.
However, an additional question may be worth exploring:
Could underlying metabolic dysfunction influence reward-driven behavior?
A Biological Layer Worth Considering
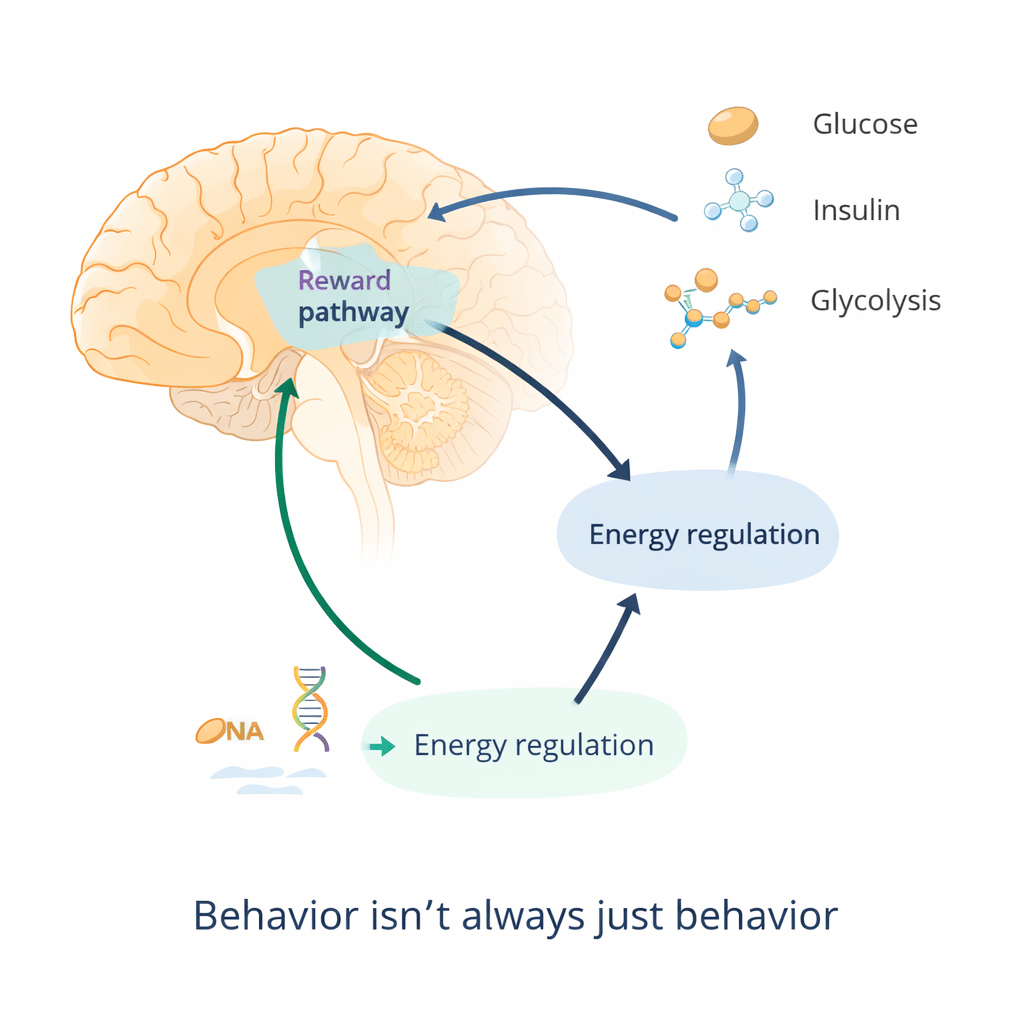
Emerging research has begun to explore the relationship between energy regulation, glucose metabolism, and the brain’s reward systems.
In particular, dopaminergic pathways—central to motivation, reinforcement, and craving—appear to be influenced by metabolic signals, including insulin activity and cellular energy availability.
In states of metabolic dysregulation—such as insulin resistance or impaired glucose tolerance—the brain’s ability to regulate reward signaling may be altered.
This raises a broader question:
Might some forms of addictive behavior represent, in part, a dysregulated energy-seeking process?
Extending the Model
If such a connection exists, it could extend beyond alcohol use to other reward-driven behaviors, including:
- Substance use (e.g., stimulants)
- Behavioral addictions (e.g., gambling)
- Compulsive reward-seeking patterns
This does not replace behavioral or psychological models.
Rather, it suggests that behavior may be influenced by underlying biological conditions that are not always visible or routinely assessed.
Why This Matters in Healthcare
Healthcare professionals operate in environments characterized by:
- Chronic stress
- Irregular schedules
- Sleep disruption
- Variable nutrition
All of which can influence metabolic health.
If metabolic dysfunction contributes—even partially—to reward dysregulation, it may represent an underappreciated factor in both vulnerability and recovery.
Implications for Thought and Practice
At present, this remains an evolving area of inquiry.
But if validated, this perspective could broaden how we think about:
- Risk assessment
- Prevention strategies
- Treatment approaches
Moving toward a more integrated model that includes:
- Biological
- Psychological
- Environmental
factors working together.
A Broader Perspective
The goal is not to replace existing frameworks.
It is to expand them.
Understanding behavior—especially in high-stakes professions—may require looking beyond what is immediately observable and considering the systems that operate beneath the surface.
Selected References & Emerging Areas of Interest
While this concept is still developing, areas of active investigation include:
- The relationship between insulin signaling and dopaminergic activity
- The impact of glucose regulation on reward pathways
- Observed behavioral changes associated with GLP-1 receptor agonists
- Broader links between metabolic health and neuropsychiatric conditions
Readers are encouraged to explore the evolving literature in these areas as research continues to mature.
Final Thought
As the conversation around wellness in healthcare continues to evolve, it may be worth asking:
Are we fully accounting for the biological systems that may shape behavior?